Otomycosis: Symptoms, Causes, and Treatment

Otomycosis is a fungal infection in the outer ear and causes inflammation, dry skin, and a smelly discharge in the ear canal. It usually affects the outer ear canal that starts from your eardrum and continues to the outside of your head. In some cases, it may affect the middle ear as well. About 10% of outer ear canal infections are caused by fungi.
Signs and Symptoms of Otomycosis

These indications typically occur in one ear, but it is possible that both ears can be affected at the same time. Typical symptoms of otomycosis include:
- A feeling of fullness in the ear
- Pain and redness of the outer ear
- Itching due to fungal infections
- Flaky skin
- Ringing in the ears
- White or yellow discharge from the ear
- Inflammation or swelling
- Hearing loss, which can be mistaken for deafness
- Redness in the outer ear
Otomycosis can become chronic if someone does not respond to treatment or has a weakened immune system, diabetes mellitus, or a chronic skin condition, such as eczema.
What Causes Otomycosis?
- Fungi. There are many different types of fungi that cause this condition. The most common fungi that cause these fungal infections are Aspergillus and Candida.
- Antibiotic and steroid use. There has been an increase in otomycosis cases in recent years. In addition to antibiotic ear drops, broad-spectrum antibiotics and steroids are believed to be responsible for this increase.
- Weakened immune systems. People with weakened immune systems are more likely to suffer from it. They may have more complications and recurrences of otomycosis. Infections that spread to the temporal bone of the skull can cause severe complications. If not treated, this can be fatal.
The Risk Factors of Otomycosis
- Using cotton swabs to clean your ears and injuring your ear canal
- Using hearing aids or earplugs, especially if you don’t clean them properly
- Getting water in your ear when swimming
- Irritants like hair dye or hair spray get in your ear
Diagnosis of Otomycosis
Symptoms of otomycosis should always be evaluated by a doctor in order to get the correct diagnosis and treatment. The doctor will take a thorough medical history to determine if any risk factors are present. They will perform a physical exam with an instrument called an otoscope to look inside the ear canal and eardrum. In some cases, a sample of cells or fluid from the ear will be taken to be examined under a microscope. This will help them to differentiate between a fungal or bacterial infection.
Treatment and Management of Otomycosis
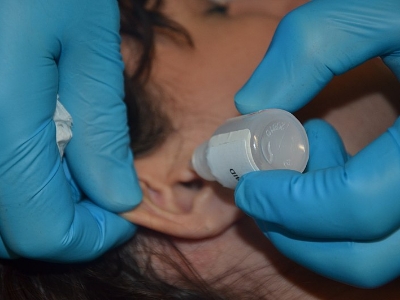
- Cleaning. Your doctor can thoroughly clean your ears to remove buildup and discharge. They may use rinses or other methods to clean your ears. Avoid using cotton swabs or other instruments inside your ears. Cotton swabs should only be used on the outside of the ear.
- Ear drops. You may need to use antifungal ear drops to treat otomycosis. Usually, a 2% solution of these ear drops is used several times a day for about a week.
- Oral medications. Some fungal infections such as Aspergillus may be resistant to the usual ear drops. They may require oral medications or you may also be advised to take over-the-counter medications such as nonsteroidal anti-inflammatory drugs for the pain.
Medication Used for Otomycosis
Clotrimazole Cream. It is an antifungal medication used as a topical treatment for tinea infections. Use this cream two or three times daily. Continue to use the cream for at least 14 days after your symptoms have gone. Ensure to finish the treatment course to get the most benefits.
Tips to Prevent Otomycosis
- Using earplugs when swimming to keep water out
- Using a hairdryer on low speed to dry ears, being careful not to burn the skin
- Leaving a small amount of earwax in the ears for its natural anti-fungal properties
- Avoiding putting cotton swabs in the ears
- Drying the ears well after swimming and bathing
- Avoiding scratching the ears as this may damage the skin and make it easier for a fungus to invade



