Hives: Symptoms, Causes and Treatment
Hives are a skin reaction that causes itchy welts. It often starts as itchy patches that turn into swollen welts that vary in size. These swellings appear and fade at random as the reaction runs its course. Chronic hives can be very uncomfortable and interfere with sleep and daily activities.
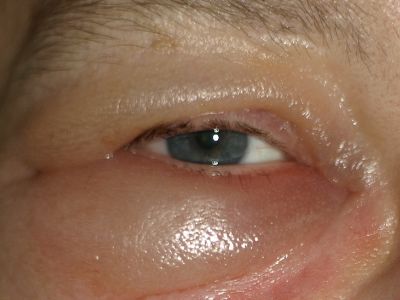
Signs and Symptoms?
- Batches of swellings can arise anywhere on the body
- Ridges that might be red, purple or skin-coloured
- Swellings that vary in size
- Welts that appear and fade repeatedly
- Itchiness which can be intense
- Painful swelling around the lips, cheeks, and eyes
- Flares triggered by heat, exercise or stress
- Symptoms that persist for more than six weeks and recur often
See your healthcare provider if you have severe conditions that last for more than a few days. Seek emergency medical care if:
- Chronic rashes do not put you at sudden risk of a serious allergic reaction
- If you get this condition as part of a severe allergic reaction
- You experience dizziness, trouble breathing
- You experience severe swelling of the tongue, lips, mouth or throat
What Causes Hives?
The swellings that come with this reaction are caused by the release of immune system chemicals, such as histamine, into your bloodstream. The specific cause of this condition depends on their type such as:
- Physical urticaria. These are caused by something that stimulates the skin such as cold, heat, vibration, pressure, sun exposure, sweating, or exercise. It usually occurs right where the skin was stimulated and rarely appears elsewhere.
- Dermatographism. This is a common form of physical urticaria where swelling or rashes form after firmly stroking or scratching the skin. It can also occur along with other forms of urticaria.
- Acute urticaria. These are rashes that last less than 6 weeks. The most common causes are foods, medications, and infections. The most common foods that cause rash are nuts, chocolate, fish, tomatoes, eggs, fresh berries, and milk.
- Chronic urticaria. These are conditions that last more than 6 weeks. The cause is usually harder to identify than those causing acute urticaria. In some cases, the cause may be thyroid disease, hepatitis, infection, or cancer.
Are Hives contagious?
Unlike some other skin conditions, these are not contagious. But if you develop rashes because your skin is exposed to secretions from a plant like poison ivy, you can spread the allergenic product to others until you wash it off.
How to Diagnose Hives?
- Skin tests. Your doctor will run tests for different allergens on your skin. If your skin turns red or swells, it means you’re allergic to that substance.
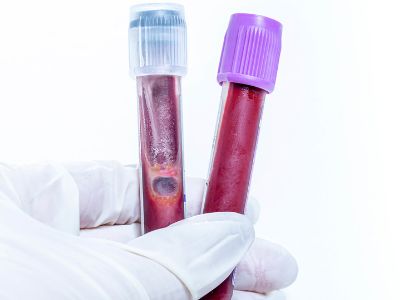
- Blood tests. It checks for specific antibodies in your blood. Your body makes antibodies to fight off allergens. If your body makes too many antibodies, you can develop rashes and swelling.
Your healthcare provider will likely talk with you about your symptoms and look at your skin. One of the effective features of this condition is that the welts come and go at random. You might be asked to keep a diary to keep track of:
- What you eat and drink
- Where hives appear and how long it takes a welt to fade
- Your activities
- Any medications including herbal remedies or supplements
- Whether your hives come with painful swelling
Treatment and Management of Hives
Treatment for chronic conditions often starts with nonprescription antihistamines. If these do not help, your doctor might suggest that you try one or more medications.
Medication Used for Hives
Loratadine. It is a medication used to treat various skin allergies. works by selectively antagonizing peripheral H1 histamine receptors. It works effectively, with the results showing immediately after taking the pill.
Lifestyle and Home Remedies for Hives
- Soothe the skin by covering the itchy area with a cold washcloth or rubbing an ice cube over it for a few minutes.
- Apply an anti-itch cream or lotion with menthol for a soothing effect.
- Avoid wearing clothing that’s rough, tight, scratchy or made from wool.
- If you think a medication caused your welts, stop using it and contact your primary care provider.
- Use a nonprescription anti-itch drug to avoid drowsiness and may help ease itching.
- Protect your skin from the sun and apply sunscreen about a half hour before going outdoors.
- Avoid triggers that include foods, medications, pollen, pet dander, latex and insect stings.



