Actinic Keratosis: Symptoms, Risk Factors, Causes, and Treatment
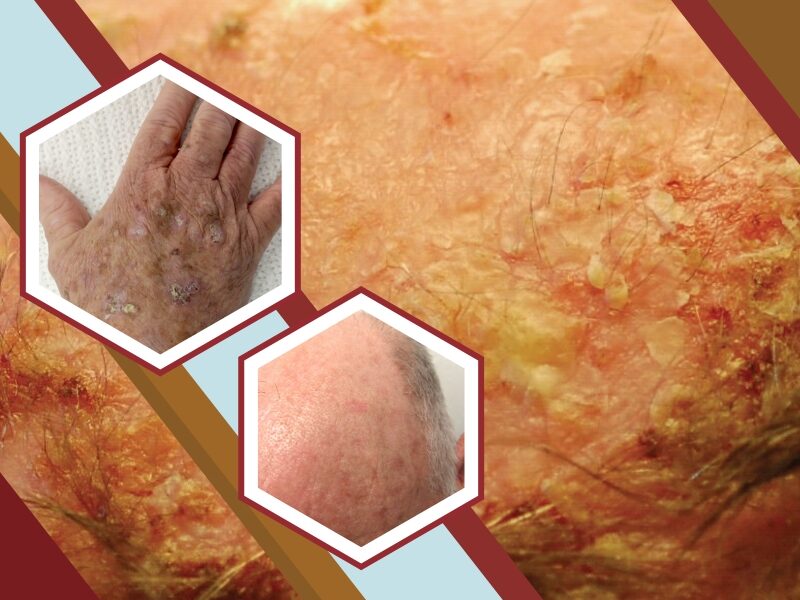
Actinic keratosis is the most common precancer that forms on skin damaged by chronic exposure to ultraviolet rays from the sun or indoor tanning. It is a rough, scaly patch on the skin that develops from years of sun exposure. It is often found on the face, lips, ears, forearms, scalp, neck, or back of the hands.
The patch on the skin grows slowly and usually first appears in people over 40. You can reduce your risk of this skin condition by minimizing your sun exposure and protecting your skin from ultraviolet rays.

Signs and Symptoms of Actinic Keratosis
- Wartlike surface
- Color variations, including pink, red or brown
- Itching, bleeding, burning, or crusting
- New patches or bumps on sun-exposed areas of the head, neck, hands, and forearms
- Rough, dry, or scaly patch of skin, usually less than 1 inch in diameter
- Flat to slightly raised patch or bump on the top layer of skin
Risk Factors of Actinic Keratosis
UV rays from the sun and from tanning beds can increase your risk of developing this condition. Damage to the skin from UV rays builds up over time and even short-term exposure to the sun regularly can build up over a lifetime and increase your risk of the condition. Other risk factors are:
- People with darker skin, hair, and eyes have been exposed to UV rays without protection.
- People with pale skin, blonde or red hair, and blue, green, or gray eyes.
- Older adults or the ones with suppressed immune systems caused by chemotherapy, organ transplant, or AIDS.
- People with rare conditions such as albinism or xeroderma pigmentosum
Causes of Actinic Keratosis
Actinic keratoses are the result of abnormal skin cell development due to DNA damage by short-wavelength UVB. They are more likely to appear if the immune function is poor, due to aging, recent sun exposure, predisposing disease, or certain drugs. The main concern is that this condition indicates an increased risk of developing cutaneous squamous cell carcinoma. It is rare for a solitary AK to evolve into squamous cell carcinoma but the risk occurring at some stage in a patient with more than 10 AKs is thought to be about 10 to 15%.
Treatment and Management of Actinic Keratosis

An AK sometimes disappears on its own but might return after more sun exposure. Your doctor may prescribe a medicated cream or gel to remove them. These products might cause redness, scaling, or a burning sensation for a few weeks. Other treatment options are:
- Scraping. It destroys the affected tissue with an electric current. This procedure requires local anesthesia. Side effects may include infection, scarring, and changes in the skin color of the affected area.
- Cryotherapy. AKs can be removed by freezing them with liquid nitrogen. As your skin heals, the damaged cells slough off, allowing new skin to appear. Side effects may include blisters, scarring, changes to skin texture, infection, and changes in the skin color of the affected area.
- Laser therapy. It destroys the patch, allowing new skin to appear. Side effects may include scarring and discoloration of the affected skin.
Medication Used for Actinic Keratosis
Imiquimod Cream is a drug that is topically administered. It is widely used to treat different types of skin infections such as AKs or minor forms of skin cancer known as superficial basal cell carcinoma and external genital warts. It improves the immune response of the cells when applied. The activated immune cells travel to areas of infection and eliminate the infected cells.
How to Prevent Actinic Keratosis?
- Limit your time in the sun, especially between 10am to 2pm.
- For extra protection from the sun, wear tightly woven clothing that covers your arms and legs.
- Avoid tanning beds because they can cause just as much skin damage as a tan acquired from the sun.
- Use sunscreen before spending time outdoors, even on cloudy days, and apply a broad-spectrum water-resistant sunscreen with a sun protection factor of at least 30.
- Apply sunscreen at least 15 minutes before going outside and reapply it every two hours or more often if you are swimming or perspiring.
- Check your skin regularly and report changes to your doctor.



